What is ERCP?
Endoscopic retrograde cholangiopancreatography (ERCP) is a diagnostic and interventional procedure that combines an endoscope and X-ray to examine and treat problems of the bile duct, pancreatic duct and gallbladder.
During the ERCP procedure, a thin, hollow, flexible tube with a camera attached at one end, known as an endoscope, is inserted into the digestive tract. The endoscope is carefully guided through the mouth and throat, then down the oesophagus, stomach, and duodenum, which is the first part of the small intestine as well as the shortest.
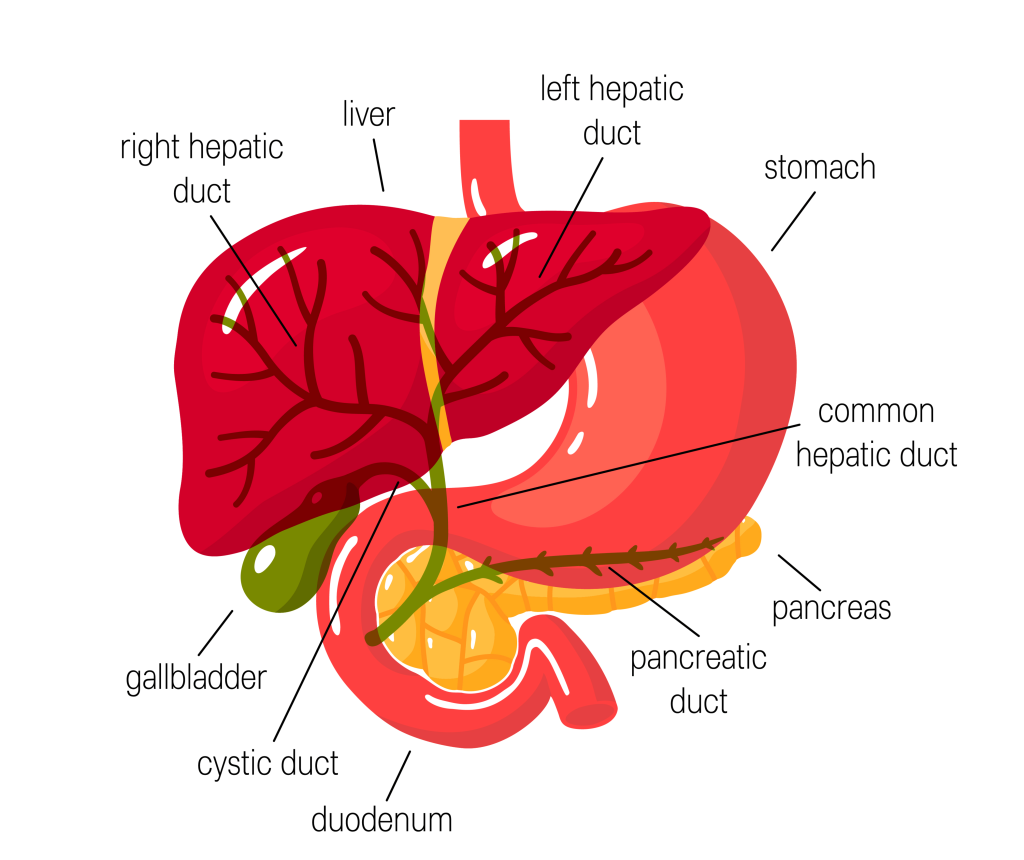
Once the endoscope reaches the duodenum, the papilla (ampulla of Vater) is located to cannulate it. The papilla serves as the point where the common bile duct and pancreatic duct enter the duodenum.
At the papilla, a small flexible tube called a guidewire is passed down the endoscope and into the papilla to reach the bile duct and pancreatic ducts. A dye is then injected into the ducts, and X-ray images are captured as the dye causes these various passages to light up on the X-ray.
- Bile ducts — These thin, long tubes connect the liver, gallbladder, and pancreas to the duodenum and carry bile to the gastrointestinal tract.
- Pancreatic ducts — These ducts drain pancreatic fluid from the pancreas and carry it to the duodenum.
While the ERCP procedure is relatively safe, roughly 5-10% of these procedures may be associated with certain complications, such as:
- Pancreatitis (most common complication)
- Pain
- Infection
- Bleeding
- Abnormal reaction to the sedative used
- Damage or rupture to surrounding structures
Why Do I Need the ERCP Procedure?
Certain presentations may be an indication for to carry out an ERCP. These include, but are not limited to:
- Patients presenting with jaundice
- Symptoms include yellow skin/eyes, pale stools, and/or dark, tea-coloured urine.
- Causes include gallstones, strictures, tumours, trauma and injury to the bile duct, and sphincter of Oddi dysfunction
- Patients in whom hepatobiliary tract abnormalities are highly suspected
Diagnostic purposes
The ERCP procedure is beneficial in evaluating and diagnosing problems in your biliary system, including:
- Biliary tract abnormalities
- Dilation of the pancreatic duct
- Bile duct obstruction (causes include gallbladder stones)
- Evaluating narrowed segments, also known as strictures, of the bile ducts
- Cancer in the liver, pancreas, or gallbladder
- Infections of the bile ducts
- Diagnosing conditions such as primary biliary cholangitis or primary sclerosing cholangitis
- A sample of tissue may also be removed (biopsy) during the ERCP to be sent to the lab for further analysis by a pathologist
Therapeutic purposes
ERCPs can be used to treat certain conditions of the bile ducts and pancreatic ducts. In certain cases, it may also be used before or after gallbladder surgery. For instance, if any complications involving the bile duct arise or are suspected, the ERCP procedure can be used to address these issues, enhancing the overall ease and success of the treatment.
ERCP is involved in the treatment of many conditions, including:
- Gallstone extraction
- Insertion of a stent to relieve blockage
- Dilation of strictures
- Endoscopic sphincterotomy (opening up the entry of the ducts into the bowel)
- Drain blocked areas
Dr Benjamin Yip, the Medical Director and Consultant Gastroenterologist of Alpha Digestive & Liver Centre, shares: “Although ERCP is one of the higher-risk endoscopic procedures, it is usually well-tolerated. I had a patient in her 90s with incurable ampullary cancer on whom I performed the ERCP procedure and inserted a biliary metal stent to prevent biliary blockage. I remember seeing her one year following the ERCP. She was doing well, and the stent was functioning well, too!”
Is the ERCP procedure Considered Surgery?
Endoscopic retrograde cholangiopancreatography is considered a minimally invasive procedure, which means the approach taken is considered low-risk with minimal damage to surrounding body tissues.
Can the ERCP procedure Be Used to Remove Gallstones?
It can be used to remove stones in the bile duct and pancreatic duct but not those from the gallbladder.
ERCP vs MRCP
Although the ERCP procedure is commonly used by many Gastroenterologists and other specialists, it is not free of complications. This makes Magnetic resonance cholangiopancreatography (MRCP) a suitable alternative option to assess and diagnose problems in the bile and pancreatic ducts. The main difference between the two is that MRCP can only be used for diagnostic purposes, whereas ERCP can also be used for therapeutic purposes. Nonetheless, both procedures are very helpful in managing patients.
Unlike ERCP, which uses radiation (X-rays), MRCP uses a powerful magnetic field and radio waves to produce detailed images of the hepatobiliary system and pancreatic system. Procedure-wise, the patient will be asked to lie down still within the MRI machine while it generates a magnetic field around the patient to produce the images. In some hospitals, straps may be fastened to hold the patient in place. You will not feel anything during this process, and it usually takes around 20 minutes to complete, but in some cases, it may take longer. As the machine can be quite loud, earphones or headphones may be provided to you. No contrast dyes are used with this test, but if it is combined with a standard MRI, the dye may be administered intravenously (IV).
ERCP, on the other hand, involves inserting an endoscope into the mouth of the patient all the way up until the pancreas. The gastrointestinal tract is visualised with the video camera on the endoscope. Contrast is also used together with X-ray imaging.
How Do I Prepare for My ERCP Procedure in Singapore?
- Before going for ERCP, inform your care team about any allergies or medical conditions that you have, as well as your detailed medication list and whether or not you are pregnant.
- Generally, you will be asked to fast for at least 8 hours before your procedure.
- Make plans to have someone drive you home after the procedure because driving is discouraged within 24 hours of ERCP as the effects of the sedation can persist for several hours after the procedure.
What can I expect from the ERCP procedure?
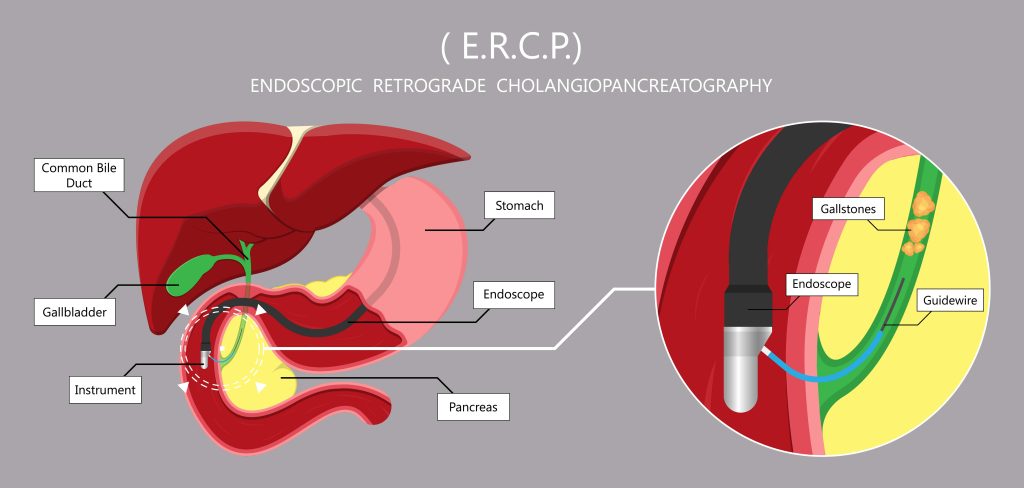
The ERCP procedure usually takes between 1-2 hours. Patients who undergo the procedure will usually have an intravenous plug set onto their arm to help with administering the sedative and other medication. A liquid anaesthetic will also be given to numb the throat and prevent gagging. A mouthguard might also be employed to facilitate the entry of the endoscope. The procedure is done lying on the left or the stomach face-down (prone position).
Once the patient is under sedation, an endoscope is inserted into the mouth and guided down the oesophagus, stomach and into the duodenum (first part of the small intestine). Once the endoscope reaches the papilla (where the common bile duct and the pancreatic duct converge and release their secretions into the duodenum), a thin, flexible guidewire is pushed through the endoscope and into the duct.
A special dye is then injected into the bile duct and pancreatic ducts to make the ducts more visible on the X-ray. A type of X-ray imaging, called fluoroscopy, is then employed to examine the ducts and to check for any blockages, narrowed areas, or masses.
If the ERCP procedure is done for therapeutic purposes, the doctor may pass small tools through the endoscope to help with the treatment. The tools employed can help carry out numerous functions, including removing stones, taking a biopsy, opening up narrowed segments, and stent insertion.
Post-ERCP
After the ERCP, you will be brought to a recovery room to rest for 1-2 hours so that the effects of the sedation and anaesthesia wear off. Most patients would be required to stay overnight in the hospital.
Common side effects include bloating, nausea, and sore throat post-ERCP. However, these should subside within a few days. Overall, the discomfort from ERCP should be mild, and patients might have little memory of the test due to sedation.
Some complications may occur following the ERCP procedure. Here are some warning clues:
- Severe abdominal pain
- Bleeding from the rectum
- Black stools
- Fever
- Jaundice
- Coughing up blood
- Nausea or vomiting that does not subside within a few days
Seek medical attention immediately if you experience any of these symptoms.
Summary
All things considered, ERCP is a safe procedure that can be used to diagnose and treat various abdominal conditions. It is a safe alternative to surgery, and it allows for a wide breadth of medical care and treatment. If you would like to learn more about how ERCP can help or have any symptoms that have been mentioned above, get in touch with us at Alpha Digestive & Liver Centre. Our team will schedule an appointment with our experienced Consultant Gastroenterologist, Dr Benjamin Yip, who will guide you with all your questions and concerns.
Dr Yip is one of the few ERCP experts in Singapore. He was honoured with the Health Manpower Development Plan award to sub-specialise in Advanced Endoscopy at the Royal Free and University College Hospitals in London, UK. Throughout his time there, he underwent training under prominent leaders in the Advanced Endoscopy field, honing his skills in ERCP and other types of specialised endoscopies.
References
- ASGE | Understanding ERCP, https://www.asge.org/home/for-patients/patient-information/understanding-ercp. Accessed 10 May 2022.
- “Endoscopic Retrograde Cholangiopancreatography (ERCP).” Johns Hopkins Medicine, https://www.hopkinsmedicine.org/health/treatment-tests-and-therapies/endoscopic-retrograde-cholangiopancreatography-ercp. Accessed 10 May 2022.
- “Endoscopic Retrograde Cholangiopancreatography (ERCP) | NIDDK.” National Institute of Diabetes and Digestive and Kidney Diseases, https://www.niddk.nih.gov/health-information/diagnostic-tests/endoscopic-retrograde-cholangiopancreatography. Accessed 10 May 2022.
- ERCP. UCSF, Surgical Oncology Program, https://surgicaloncology.ucsf.edu/conditions--procedures/ercp.aspx. Accessed 4 March 2024.
- ERCP (Endoscopic Retrograde Cholangiopancreatography). Cleveland Clinic, https://my.clevelandclinic.org/health/diagnostics/4951-ercp-endoscopic-retrograde-cholangiopancreatography. Accessed 7 March 2024.

