Gastroscopy in Singapore – How is it performed?
A gastroscopy or Oesophago-Gastro-Duodenoscopy (OGD) is a common procedure in Singapore that examines the upper gastrointestinal (GI) tract, which includes the oesophagus, stomach, and upper part of the bowel using a medical instrument called a gastroscope or an endoscope. This procedure helps in the diagnosis of medical conditions such as peptic ulcers and gastritis.
How far into my digestive system does an OGD go?
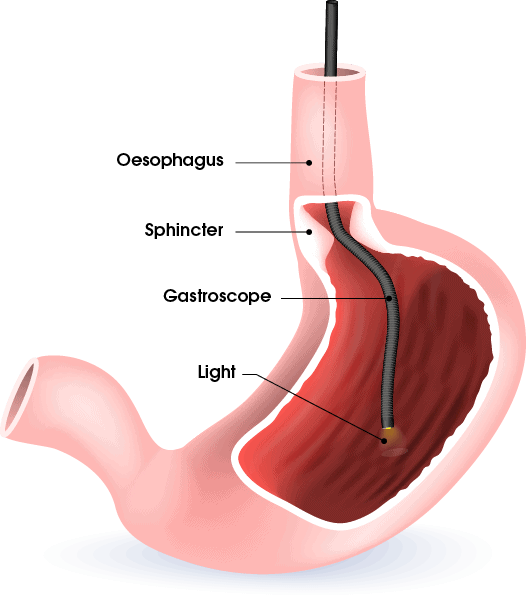
As the name suggests, an Oesophago-Gastro-Duodenoscopy (OGD) travels from the mouth to the duodenum, which is the first part of the small intestine.
What is a Gastroscopy required for?
Your gastroenterologist may recommend that you carry out a gastroscopy in Singapore for diagnostic or therapeutic purposes.
The purpose of diagnostic Gastroscopy includes:
- The inspection of the upper gastrointestinal tract for benign or malignant lesions, diffuse mucosal changes and luminal obstruction.
- Photography or video-recording of the organs.
Common therapeutic Gastroscopy procedures include:
- Biopsy of tissue samples
- Dilation of strictures
- Stent placement
- Removal of foreign bodies and lesions
- Placement of feeding tubes e.g. percutaneous endoscopic gastrostomy tubes
- Treatment of upper GI bleeding
Who needs a Gastroscopy?
Gastroscopy is generally performed if you have the following symptoms:

Suspected cancer of the oesophagus or stomach

Suspected gastric or oesophageal ulcer

Chronic or persistent nausea, vomiting, or heartburn

Upper abdominal discomfort and pain

Dysphagia or odynophagia (difficulty swallowing)

Anorexia and unknown weight loss

Black stool or blood in stool
What are the common conditions that can be diagnosed using a Gastroscopy?
- Gastroesophageal reflux disease (GERD)
- Helicobacter pylori
- Gastritis
- Gastric polyps
- Peptic ulcer disease (gastric/duodenal ulcers)
- Barrett's oesophagus
- Coeliac disease
- Portal hypertension
- Cirrhosis
- Hiatal hernia
- Oesophageal cancer
- Stomach cancer
How do I prepare for a Gastroscopy in Singapore?
Prior to a gastroscopy, a general examination of your health, medical allergies, ability to tolerate the procedure, and reactions to sedation will be conducted.
- Your gastroenterologist will also explain the details of the procedure, including any associated risks.
- You will be informed about the medications that should be stopped temporarily. Do let the doctor know if you are on any blood thinners, sedatives or diabetic medication.
- You will also be asked to fast for at least six hours prior to the procedure. This is to ensure that the stomach is empty for clear visualisation of the structure. But you can drink a few sips of water up to two hours before your appointment.
- As a sedative may be given during the gastroscopy, it is advisable to arrange for private transport or someone to pick you up from your gastroscopy clinic in Singapore after the procedure.
Are there any risks associated with a Gastroscopy in Singapore?
Gastroscopy in Singapore is generally well-tolerated and safe, but it does carry some risks. The possible risks associated with gastroscopy include:
- Bleeding — Some bleeding may occur during the biopsy, which will usually stop on its own. Otherwise, do consult the doctor to stop the bleeding.
- Sore throat — This is a common side effect of the procedure and may last a few days. However, do consult the doctor if you experience severe pain in the throat, chest, or abdomen.
- Infection — After a biopsy, there is a very small chance that the wound might become infected. Do consult your gastroscopy clinic in Singapore if you experience any fever, cold, or are feeling generally unwell. A chest infection may occur from secretions entering the airway due to the throat being numb or from sedation. This can be prevented by suctioning the secretions during the procedure.
- Damage to teeth — The insertion of the gastroscope into the mouth may cause some damage to the teeth. The use of the mouthguard during the procedure will help prevent this from happening.
- Reaction to sedation — Sedation may affect breathing, heart rate, and blood pressure. During the procedure, you will be monitored closely and treated appropriately if any complications from sedation arise.
- Perforation — The gastroscope may cause a tear in the lining of the oesophagus, stomach, and duodenum and will require surgery to repair.
Rest assured, OGD’s are the most common procedures performed by gastroenterologists. They have a very low risk and, on average, take about 10 minutes to complete. According to Dr Benjamin Yip, patients can generally leave the hospital half to one hour after the procedure. For selected patients, this procedure can even be done without sedation!
What can I expect during my Gastroscopy in Singapore?

Sedatives
Before the gastroscopy begins, your mouth and throat will be numbed with an anaesthetic gargle or spray. Any removable dentures will also be taken out.
If you choose to be sedated, a light sedative will be administered intravenously making you go into a sleep-like state for a short period of time.
Due to the use of sedatives, adequate monitoring for safety in the form of pulse oximetry, blood pressure, and visual cues of respiratory rate and effort will be performed.
General procedure
You will be placed in a left lateral decubitus position, which means that you will need to lie on your left side. A protective ring or a bite block is placed between the teeth to ensure that your mouth remains open during the procedure and to allow easy gliding of the gastroscope.
You may be asked to perform several swallows to aid the gastroscope in entering the oesophagus. It is inserted gently into your mouth and then slowly passed into the stomach and the duodenum.
During the procedure, a small amount of air may be delivered to visualise the oesophagus and stomach clearly.
The oesophagus and stomach linings are examined for any abnormalities such as redness, inflammation, bleeding, and ulcers. A tissue sample may also be obtained for further evaluation. Certain medical conditions, such as bleeding and narrow passages, may also be treated during your gastroscopy in Singapore.
Tissue sampling and excision
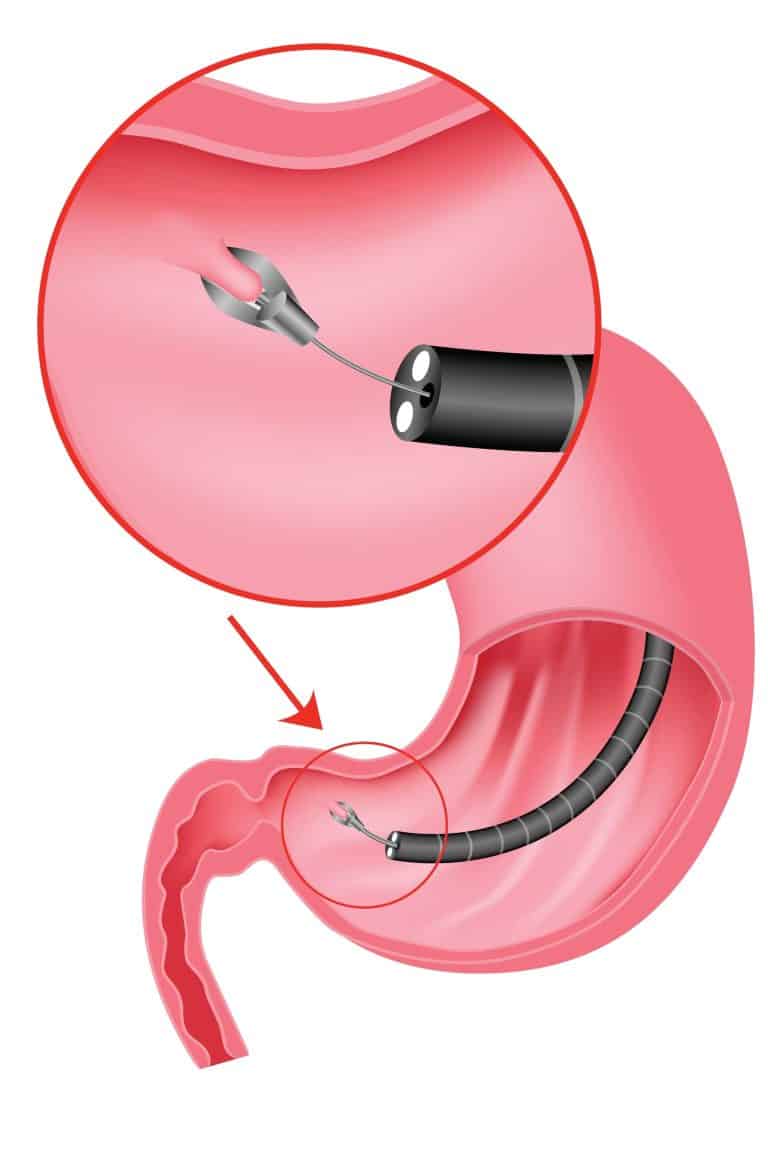
Therapeutic procedures
A variety of small instruments are able to pass through the gastroscope in various therapeutic interventions such as tissue sampling and excision, bleeding control, and dilatation or stenting of strictures.
Tissue sampling and excision
- Superficial biopsies limited to the mucosa involve the use of standard biopsy forceps. An endoscopic mucosal resection (EMR) is a technique employed to obtain bigger and deeper biopsies of benign masses.
- Larger lesions beyond the size of the EMR device can be excised by endoscopic submucosal dissection (ESD).
Bleeding control
- Multiple tools can be used for bleeding control, and they are categorised as injection, thermal, and mechanical therapy. In addition, topical agents may also be utilised. The goal of the injection therapy is to provide haemostasis through the tamponade and vasoconstricting effect due to the injected substance, such as diluted epinephrine or saline.
- Thermal therapy involves the delivery of energy-inducing direct tissue coagulation, contraction, and desiccation. Mechanical therapy uses the standard through-the-scope endoscopic clips that help to provide superficial vessel closure and closure of perforation.
Dilatation or stenting of strictures
- Gastric outlet obstruction can be caused by benign or malignant lesions. Balloon dilatation may be used for benign strictures which involve the inflation of the balloon through the catheter to a specific size. For unresectable or metastatic disease, a self-expanding metal stent (SEMS) will be considered with palliative intent.
Time
The procedure typically lasts about 10 to 15 minutes.
Equipment
The main equipment involved in this procedure is the endoscope. The endoscope is a long, thin, flexible tube that has a light and video camera attached at one end. The video camera captures images that are transmitted to the doctor's screen for viewing. The endoscope also has a channel for insufflation and water. Most importantly, it is equipped with an instrument channel where therapeutic modalities can be delivered.
What can I expect after a Gastroscopy in Singapore?

Aftercare
If your gastroscopy is done under local anaesthesia, you may be discharged shortly after the procedure.
However, you may be monitored in the recovery area for about an hour if you have received sedation. You will be advised to avoid driving and have someone accompany you home. You should also avoid operating machinery, driving, drinking alcohol, and carrying out essential tasks like signing important documents 24 hours after sedation. If you have not received any specific instructions from your doctor, you may resume your regular medication routine once the procedure is complete.
Side effects and complications
You may experience a numb feeling in the mouth or sore throat due to the anaesthetic spray, which typically wears off after an hour. You may also experience some bloating and discomfort hours after the procedure.
Damage to the teeth may occur from the insertion of the gastroscope. In very rare cases, bleeding and injury to organs may occur during the procedure. Do consult the doctor immediately if you experience the following symptoms after the procedure:

Fever

Vomiting

Weakness and dizziness

Blood in stools or coloured stools

Shortness of breath

Severe chest pain or stomach pain

Difficulty or pain in swallowing
Who is eligible for a Gastroscopy in Singapore?
While this is a safe and effective procedure and can be performed on many patients, there may be instances where a gastroscopy is not suitable. For instance, patients who have significant respiratory problems or are unable to lie flat for an extended period may need to seek an alternative option. But whether you are suitable or not for the procedure needs to be determined by an experienced medical professional.
Summary
Gastroscopy is a minimally invasive and common procedure with both diagnostic and therapeutic capabilities. Hopefully, this guide has helped you understand what to expect from a gastroscopy in Singapore should you require one. If you have any questions or concerns, do not hesitate to reach out to our friendly staff, who will assist you with any queries that you may have.
References
- What happens during a gastroscopy? (2015, June 30). Retrieved from https://www.ncbi.nlm.nih.gov/books/NBK310264/
- Early, D. S., Ben-Menachem, T., Decker, G. A., Evans, J. A., Fanelli, R. D., Fisher, D. A., Fukami, N., Hwang, J. H., Jain, R., Jue, T. L., Khan, K. M., Malpas, P. M., Maple, J. T., Sharaf, R. S., Dominitz, J. A., & Cash, B. D. (2012). Appropriate use of GI Endoscopy. Gastrointestinal Endoscopy, 75(6), 1127–1131. https://doi.org/10.1016/j.gie.2012.01.011
- Gastroscopy. Gastroscopy | Tests and Scans Cancer Research UK. (2019, March 15). Retrieved from https://www.cancerresearchuk.org/about-cancer/cancer-in-general/tests/gastroscopy
- Li, C., & Ellsmere, J. (2019). Diagnostic and therapeutic endoscopy of the stomach and small bowel. Shackelford's Surgery of the Alimentary Tract, 2 Volume Set, 647–662. https://doi.org/10.1016/b978-0-323-40232-3.00057-1
- After Your Gastroscopy at Toronto General Hospital. Health information. (2019, June). Retrieved from https://www.uhn.ca/PatientsFamilies/Health_Information
- Murdoch & Perth. Conditions Detected by a Gastroscopy or a Colonoscopy https://www.wexfordgastro.com/conditions-diagnosed-using-endoscopy-murdoch-perth/
- Ali A Alali, Alan N Barkun. An update on the management of non-variceal upper gastrointestinal bleeding.
- https://academic.oup.com/gastro/article/doi/10.1093/gastro/goad011/7081277


